It started with a rash, a rash that would not go away. I was 20, as far as the healthcare system was concerned, an adult old enough to make my own decisions. I called my primary care doctor’s office and set up an appointment. The doctor checked the rash out, wrote a prescription, and asked me if I wanted to see a dermatologist. A specialist for a persistent rash, sure, why not? The earliest date that I could get an appointment was 4 weeks out.
My first surprise was at the pharmacy where I went to collect the medicine. The prescribed steroid cream cost $200 out of pocket. A few weeks later, I had my appointment with the dermatologist. She wanted to do a rash evaluation and find out if the rash was fungal, bacterial, or viral. She did a skin biopsy, looked at it under a microscope, and ruled out fungus. She said she would send the bit of skin to the lab to test for bacteria or viruses. She wrote out a prescription for another topical steroid. At the pharmacy, I was told that this prescription would cost $150 out of pocket. I called the doctor’s office and asked if they could prescribe an alternative that cost less. They changed it to an oral steroid that cost $5.
I waited a week and still had not heard back from the lab. I called the doctor’s office and they said that the tests had come negative – it was neither bacterial nor viral. A few weeks later my mother received an itemized bill for $1333.

$250 for the fungal test, $250 for the bacterial test, $250 for the viral test, $250 for the primary care doctor, and $333 for the specialist. Altogether, I (well, my mom) had paid $1538 and I still had the rash. If I had not made the phone call and got the prescription changed, my mom would have ended up paying $1683 for a rash that was still there.
My dad heard about this and sent me two creams – Betnovate-N and Betnovate-C, with the instructions – if these are heat blisters, apply N; if the rash is because of humidity, apply C. These are over-the-counter topical steroids that he regularly gets on his visits to India.

The rash was on the sole of my foot, thinking maybe the sweat inside my shoes was keeping it humid – I applied C. I was rash-free in days. The cost of the two tubes – ₹100, which is about $1.25. It would have cost me less to fly to India, buy the creams and come back.
It’s the Prices, Stupid
In a widely cited article published in 2003 in Health Affairs [1], snarkily titled “It’s the Prices, Stupid”, the authors used data from the Organization for Economic Cooperation and Development (OECD) and concluded,
In 2000 the United States spent considerably more on health care than any other country, whether measured per capita or as a percentage of GDP. At the same time, most measures of aggregate utilization such as physician visits per capita and hospital days per capita were below the OECD median. Since spending is a product of both the goods and services used and their prices, this implies that much higher prices are paid in the United States than in other countries. But U.S. policymakers need to reflect on what Americans are getting for their greater health spending. They could conclude: It’s the prices, stupid.
In 2019, the authors reiterated the assertion in an article published in Health Affairs [2], titled “It’s Still The Prices, Stupid”. To understand their argument, let’s formalize that into a formula.

They argue that since the US spends much more on health care (per capita) and is below the median on units of goods and services, the explanation has to be that prices are higher. In the formula, if CHC is higher than the OECD median, and N (total units of care used) is below the median, then the only explanation is that the unit price (p) must be much higher in the US.
Is that really true? In my case, $450 was what I spent for the care, the rest $1088 ($1538 – $450) would typically be classified under over-treatment. Out of the $1138, $750 can be classified as unnecessary tests.
The other issue is the cost of prescription drugs. Betnovate is a broad-spectrum drug with anti-bacterial, anti-fungal and anti-inflammatory properties. Patients want their health concerns addressed. They don’t want to be tested like guinea pigs and then charged for the testing. Why isn’t a broad-spectrum medication the first line of treatment for a rash?
The treatment that you get and the drugs that you are prescribed are controlled by algorithms that factor in the insurance that you are on and where you are on your out-of-pocket payments. Prescription drug prices are controlled by pharmacy benefit managers (PBM), middlemen who control the formulary – the list of prescription drugs covered by a plan. The top three PBMs today control over 80% of the market giving them extreme control over recommending drugs and setting their prices.
Let’s make an adjustment to the formula to break up the components of the price of care.
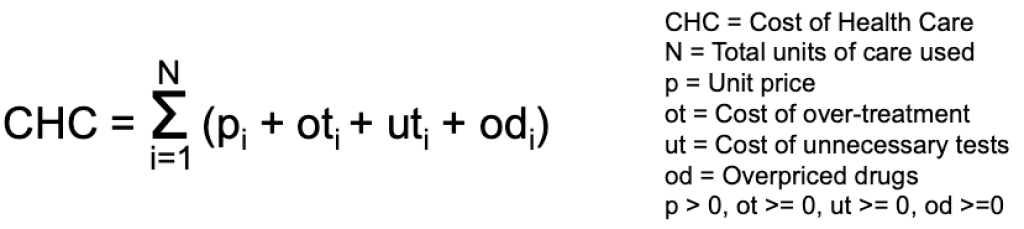
In all fairness, the over-treatment, unnecessary testing, and overpriced drugs are not a function of the healthcare system but a function of the insurance that I was on. To understand why the insurance determined the treatment, we must first understand the various types of health insurance product options.
The Value of Choice
People like having options. Having free will and the ability to choose is seen as a core democratic value. Having options puts us in control. We see value. Having options allows us to pick a plan personalized to our needs. Well, that’s what marketers have been telling us.
We value having choices but unfortunately choosing comes at a cost. Insurance product choice is a primary feature of all health insurance providers in the US. Individuals have to decide what plan works best for them and their families. Most employers and exchanges offer multiple options that include HMO plans, EPO plans, and several PPO high-deductible plans. For those eligible for Medicare, it is not any easier – you have to choose between regular Medicare and Medicare Advantage, choose between Medicare Advantage plans, Medicare Part D plans, and Medicaid managed care plans.
For many employees and seniors, open enrollment is a nightmare that they could do without. Many make poor choices with consequences that echo through the year. A patient’s out-of-pocket expense depends on insurance status, extent of coverage, and where they are in the deductible and coverage phase of their benefits.
You have HMO plans where all your medical costs are covered by insurance but your monthly premiums are high. If you want to reduce your monthly premium, you sign up for a high-deductible plan. The insurance starts paying costs only after the deductible is reached. If you are a fairly healthy family that needs just routine wellness checks, a high-deductible plan with an HSA or FSA plan might work.
The choice you make also determines the care you get. My mother was on a high-deductible plan. If she had been on an HMO plan, it is highly unlikely that the primary care physician would have referred me to a dermatologist for a rash.
Surveys show that most people are not confident in their ability to choose the right plan for themselves and their families. Surveys also show that cost concerns are the #1 reason (even topping COVID-19 concerns) for skipping or delaying health care. The choice we are asking for is not personalized health insurance plans. The choice we are asking for is to see the doctor we want to get the care we need at a price we can afford.
The Cost of Choice
The Organization for Economic Cooperation and Development (OECD) publishes data annually about the healthcare systems of its member countries. Has the choice to pick your personalized health insurance plan led to a reduction in total costs? Have health outcomes improved over the years? The figure below shows the trend over the years for OECD member countries.
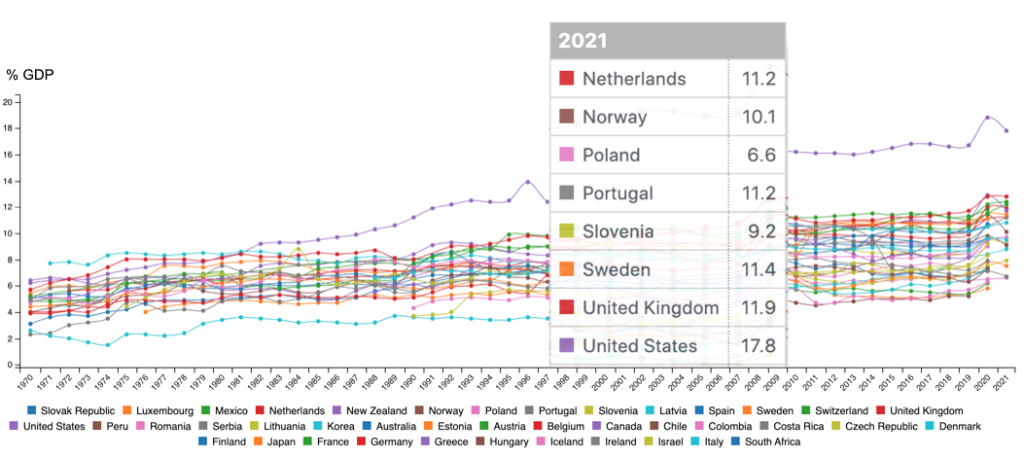
The US is clearly an outlier. In 2021, the US spent $4.3 trillion on health care which accounts for about 18% of GDP. This is around 2X the median of the OECD countries. The total health care spending and per capita both show similar trends. Starting in the early 1980s, US health care costs branch off from the rest of the countries. The 1980s is when newer care models like HMOs were introduced; consumers got more choice and the assumption was that with choice would come lower costs. The reverse has happened. Before we drill into the reasons for the disproportionate rise in costs over the years, it is important to capture all components of the cost for health care (CHC) in our formula.
Transparency in Pricing
Several years back, my dad went through a dental procedure. He was on a PPO Dental (100/80/50) plan where for a particular procedure he had to pay 50% of the costs while insurance covered the other 50%. After the procedure, he received a bill for $750 and he paid his share of $375. A few weeks later, he got an Explanation of Benefits statement from the insurance company informing him that they paid their 50% share. The statement showed the cost of the procedure as $500 and their share as $250. The dental group made $625 on a procedure which actually cost $500. This kind of fraud is enabled whenever there is a lack of transparency in pricing. Let’s modify the formula to account for fraud.
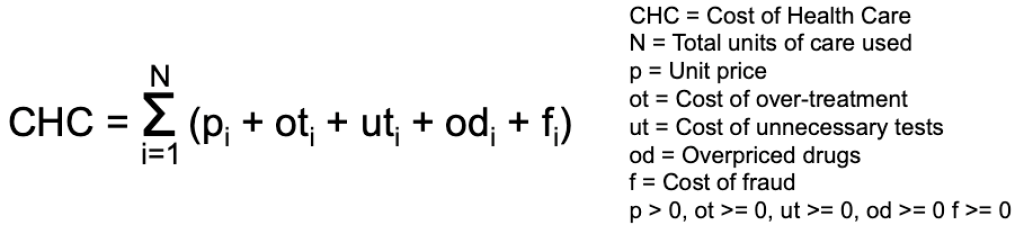
In 2019, the White House issued an executive order aimed at improving healthcare price transparency. The Transparency in Coverage Final Rule issued by the Centers of Medicare and Medicaid Services (CMS) requires healthcare providers to disclose to consumers the cost of an item or service before receiving the care. The intent of the rule was that transparency would encourage free markets, enhance competition, and allow consumers to shop around and make informed decisions.
In 2019, my mother felt a lower pelvic pain. Her doctor ordered a pelvic ultrasound – to be precise, the doctor ordered a US Pelvic and Transvaginal Non-OB test. The ultrasound did not find anything remarkable. A few weeks later, she got an itemized bill. By then, the pain had long gone but the bill made her double over.
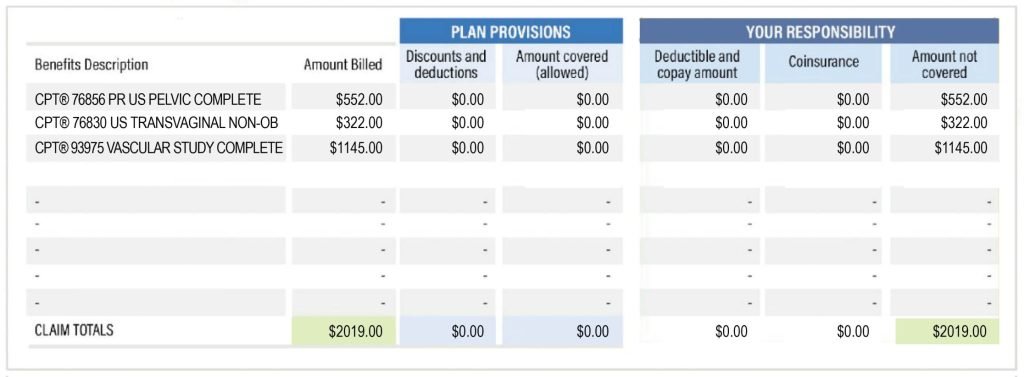
A bill for $2,019 for what turned out to be a stomach ache. My mother spent hours on the phone contesting the bill – the doctor’s office said that a vascular study was done as part of the ultrasound and passed her off to billing. The billing department claimed that they had just billed for the tests ordered. She checked her healthcare provider’s website – in accordance with the Transparency in Coverage law, they had listed prices for all services on their website. For each of the tests, she was billed exactly the price that was listed on the website.
She searched the web, researched CPT® codes, and finally drafted an email to the billing department contesting the charge for CPT® 93975, explaining that the test results did not include any reports for a full-body vascular study. Within two days of sending the email, she heard back – the billing office acknowledged that it was an error on their part and she didn’t need to pay the $1,145.
It took weeks to resolve but it was a win for her, or so she thought. It was only at the time of researching for this article that we realized that she had been a victim of not just over-coding but also unnecessary testing. If the insurance were paying the costs, they would have done their due diligence. Since we were below the deductible limit for the year, the insurance passed on the costs to us.
CMS maintains an updated list of Current Procedural Terminology (CPT®) codes. Improper coding leads to inappropriate charges and payments. The Medicare National Correct Coding Initiative (NCCI) was implemented to promote correct coding methodologies nationally. NCCI identifies individual services that are components of more comprehensive services using NCCI edits. NCCI edits are designed to promote correct coding and prevent inappropriate payments by bundling component codes into the more inclusive code. Component services that are billed separately from the more inclusive service are denied, unless an exception is specified.
The NCCI edits lookup tool is available at – https://www.cgsmedicare.com/medicare_dynamic/j15/ptpb/ptp/ptp.aspx – and the form is shown below with an NCCI edit for CPT® codes 76856 and 76830.
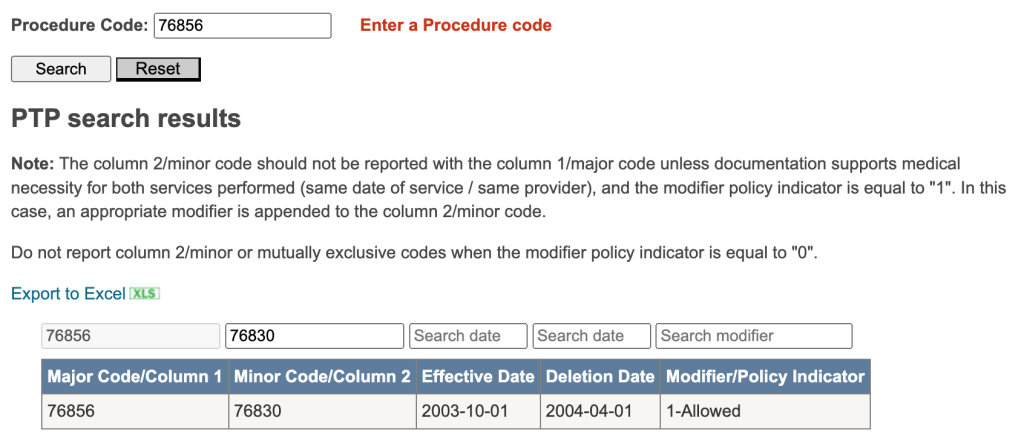
Insurance should typically act as a gatekeeper and flag over-coding. When you are on a high-deductible plan and below your deductible, the insurance has no interest in checking this and it is caveat emptor. Very few understand the medical-speak, can decode the jargon, and can advocate for themselves. NCCI edits technically apply only to Medicare fee-for-service payments but private payers routinely apply these edits to deny claims. Aetna, in its Clinical Policy Bulletin [3], includes the following note.
Pelvic ultrasound is considered to be clinically integral to the transvaginal examination and does not warrant separate reimbursement. A transvaginal ultrasound (TV-US) provides superior detail in images of pelvic structures.
An Aetna Policy Change effective December 1, 2012 states – 76856 will deny as incidental when billed with 76830 on facility claims. Specialist claims are currently subject to this edit.
In an article published in the journal Radiology [4] in 1988, the authors reviewed sonographic images of patients who underwent concurrent transabdominal and transvaginal pelvic ultrasounds. They report that transvaginal image quality was better in 79% – 87% of the scans and the techniques provided equivalent diagnostic information in 60% – 84% of the cases.
ClearHealthCosts is an online company bringing transparency to the healthcare marketplace by informing people about what procedures cost. They crowd-source data and provide a search tool that allows you to search the cost of a procedure. You can search by name or CPT® code and find costs at healthcare facilities around where you live. The figure below shows a claim [5] that was submitted to ClearHealthCosts, where one of the codes was denied because of the NCCI edit.
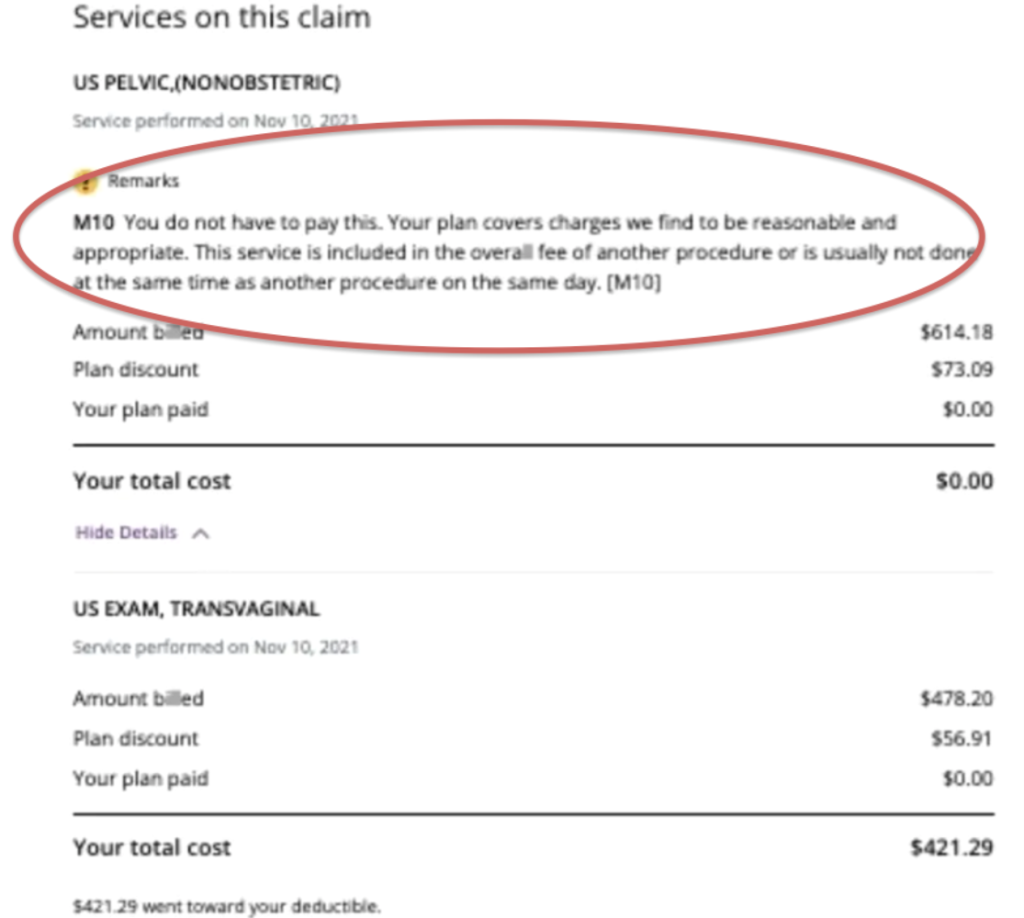
The insurance company rejected the claim for CPT® 76856 (US PELVIC NONOBSTETRIC) referring to the NCCI edit that the two codes cannot be performed on the same date (and same provider) unless there is a medical exception provided.
I was over-treated and over-tested. My mother was over-coded and over-tested. Transparency in pricing did not prevent over-testing or over-coding. High-deductible health plans have compounded the issue as insurance companies have no incentive to play watchdog when someone is under their deductible limit for the year. The high cost of health care in the US is not just the prices – it is the prices, over-treatment, unnecessary tests, fraud, over-coding, and inefficiencies encouraged by a systemic lack of incentive to innovate.

A simple suggestion that allows a patient to price-shop is to make sure that when a healthcare provider orders a test, they include a CPT® code. This will remove the ambiguity of free text and medical-speak, prevent any loss in translation errors, and assign accountability. For the Transparency in Coverage rule to be effective, CMS must consider requiring CPT® codes to be specified for any test that a provider orders.
Misaligned Incentives
A free market forces companies to innovate, improve efficiencies, and deliver products and services that customers need. This leads to improved margins and profits for the provider and better outcomes for the customer. We have made significant advances in medical treatments but the delivery of these treatments through the healthcare system has been inefficient and unaffordable. Is there an incentive for healthcare providers to innovate, reduce waste, and make the system more efficient?
In a Harvard Business Review article [6] from 2016, the authors provide the following description of Intermountain Healthcare’s effort at innovating and improving patient outcomes.
Intermountain’s American Fork Hospital had a large birthing service. About 110 of its newborns each year were borderline premature—with a 34- to 37-week gestation versus the normal 40 weeks. Often the lungs of premature babies are not fully developed, which means they can collapse. In the distant past, most of these “blue babies” died. Then clinicians learned to place a breathing tube through an infant’s mouth into its major airway and use a mechanical ventilator to keep the lungs inflated for a few weeks. This gave infants’ lungs time to mature, and mortality rates plummeted. Unfortunately, intubation and mechanical ventilation are highly invasive, and some babies suffered significant complications.
A group of obstetricians and neonatologists at American Fork Hospital argued that since borderline preemies have lungs that are almost mature, a milder intervention, “nasal continuous positive airway pressure,” which involves blowing pressurized air through the newborn’s nose, might work. In a clinical trial, intubation rates fell from 78% to 18%. The children stayed in the nursery, not the far more expensive newborn ICU. With the simpler, less invasive care, the hospital’s total operating costs for these children fell by $544,000 a year. But fee-for-service insurance payments dropped by $873,000, causing a $329,000 dip in the hospital’s operating income. The hospital also had to bear the costs of developing and implementing the change. Moreover, when Intermountain decided to deploy the new methods across all its hospitals—clearly the right thing to do for the children—that $329,000 turned into more than $5 million in annual losses.
Today, we have a healthcare system with misaligned incentives where doing the right thing always comes at a cost, and where a win for the provider always comes at the cost of the patient. A physician might want the best outcome for a patient but the healthcare provider is incentivized to keep the patient as a returning customer. It is typically a third-party and algorithms that determine the care and treatment of a patient based on their insurance and where they are on their yearly deductible.
The misalignment of incentives has also skewed the balance between generalists and specialists. A healthcare system that puts the focus on primary care and community health will have more generalists than specialists. The figure below shows that the US is clearly an outlier. It is the only country where specialists outnumber generalists by a huge margin.
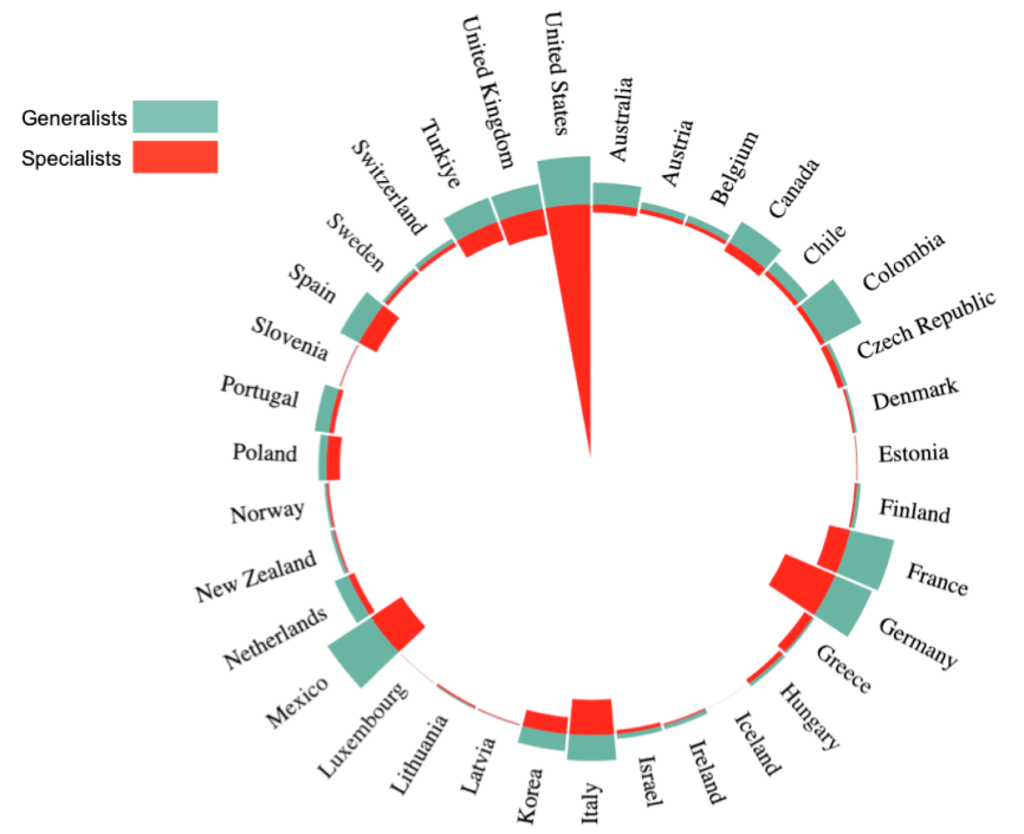
Fewer primary care doctors means less preventative care and more expensive services [7]. Long years of medical study and increasing medical school debt incentivizes medical students to gravitate towards specialities that offer higher salaries. This skew in the number of specialists has encouraged over-treatment, over-diagnosing, and perversely making patients appear sicker than they are.
The Balanced Budget Act (BBA) of 1997 established the Medicare+Choice program which introduced a variety of health plan options for Medicare recipients. Renamed as Medicare Advantage under the Medicare Modernization Act of 2003, enrollment in these plans has grown significantly since President Bill Clinton signed the BBA into law. As of April 2022, nearly 46% of all Medicare beneficiaries were enrolled in Medicare Advantage plans. Medicare Advantage was launched as a way of reducing costs. The idea was that private plans that took capitation payments per beneficiary as opposed to fee-for-service plans, would lower Medicare payments.
The flat-rate capitation payment indirectly incentivized insurance companies to create perverse schemes to sign up healthy individuals and discourage chronically ill beneficiaries. To avoid patient-selection by insurers, in 2004, CMS introduced risk adjustment, which adjusted payments based on a beneficiary’s clinical diagnoses. CMS pays Medicare Advantage providers a capitation payment per beneficiary using a complex formula called a “risk score”, which takes into account where someone lives and pays higher rates for sicker patients compared to those in good health. The program objective was to increase choice, improve quality of care, and reduce costs. Instead, costs have ballooned as private insurers figured out how to game the system – by adding diagnosis codes for chronic conditions to make patients appear sicker, which enables collecting higher payments; costing Medicare anywhere between $12 – $25 billion in over payments [8]. Legislation that tries to socially engineer a solution using fuzzy math based on an individual’s degree of health encourages insurance providers to game the system.
On November 19, 2021 the Build Back Better Act (BBBA) was passed that included provisions for lowering prescription drug prices. Drug pricing has been a black-box closely guarded by Pharmacy Benefit Managers (PBM), middlemen who profit on spread pricing. Spread pricing is the difference between the amount the PBMs reimburse the pharmacies and the amount that they charge their clients. High deductible plans have exposed these high prices to individuals. A Bloomberg report [9] analyzed 90 drugs and found that PBMs and pharmacies had siphoned off $1.3 billion of the $4.2 billion Medicaid insurers spent on drugs in 2017. It is no surprise that a generic topical steroid that costs less than a dollar outside the US, for which a pharmacy is reimbursed at probably under $10 is marked up over 2000% when charged to the client.
The Drug Price Competition and Patent Term Restoration Act of 1984 (more commonly known as the Hatch-Waxman Act) increased the availability of low-cost generic drugs while encouraging innovation by protecting new drugs with longer and stronger monopolies. While PBMs profited [10] on the spread pricing of the generics, new prescription drug prices have sky-rocketed, with list prices for rare disease drugs ranging between $750,000 to $3.5 million per dose [11]. In the last decade, data [12] shows that it is not innovation but price gouging that has driven pharmaceutical profits.
Special interest groups have already added restrictions to the number of drugs for which prices can be regulated under the BBBA, which drugs are covered, and also pushed out the year that the act will take effect. We need structural and systemic change that can address sky-rocketing drug prices and price gouging today, and not prospective legislative band-aids. Band-aids don’t fix bullet holes [13].
In the US, medical insurers operate under a general agreement called the 80/20 rule [14], where insurers are supposed to pay out 80% of the money collected from beneficiary premiums for health care claims and keep 20% for administrative, overheads and marketing costs. What is left unsaid is that the 20% includes profits. If 80% of the premiums are not paid out, the insurer has to issue rebate checks. The 80/20 rule has unintended consequences. It allows for arbitrary and high pricing to avoid paying out rebates and there is no incentive for lowering premiums. The higher the premiums, higher the 20%, higher the profits.
The Pay-for-Service model encourages over-treatment; the Capitation Payment model encourages under-treatment; the Flat-Rate Capitation Payment model encourages patient-selection; the Risk-Adjusted Capitation Payment model encourages over-diagnosis. Arbitrary rules, like the 80/20 rule, encourage arbitrary pricing and higher premiums. In the battle for the dollar between the provider and the payer, the only sure loser is the patient. The patient is left with year-to-year increasing premiums and out-of-pocket costs and year-to-year declining community health indices.
Misaligned incentives, black-box drug pricing, well-intentioned legislation that is perversely gamed by the players, and systemic and structural inefficiencies have all contributed to a dysfunctional healthcare system that rewards profits over health outcomes, prioritizes quantity over quality, and sees value in keeping the patient as a returning customer.
When healthcare providers invest in preventative care, research shows that it improves health outcomes in the long term and brings down costs. Can we create a health care model that aligns incentives towards public health and preventative care? Before we do that, let’s take a look at the data and see the effect that different payment models and health plan choice had on medical costs.
Medicare Payment Models
On July 30, 1965 President Lyndon B. Johnson signed the Social Security Amendments of 1965 into law creating Medicare and Medicaid. Hospitals and healthcare providers were paid based on a reasonable costs basis. There was no standardization of costs and hospitals and physicians had little incentive to keep prices low as they were compensated on a cost plus basis.
With program costs going up, the 1972 Social Security Amendments gave the Health Care Financing Administration (HFCA, today the Centers for Medicare and Medicaid Services (CMS)) the authority to experiment with different payment models to bring down program costs and improve the quality of health care. As a result, in the early 1980s, several HMO models were developed where the payment was on a capitation basis.
In a bid to control costs, the Social Security Amendments of 1983 introduced a new payment model for Medicare. The prospective payment system introduced codes and categories for medical procedures and established fair prices for each code and category. The fair price established the maximum price that the programs would pay for a procedure. Care services were categorized into diagnosis-related groups and claim codes and prices established. Hospitals and healthcare providers did not have any incentive to set their prices lower than the federally set maximum rate. Instead, they set their rates higher than the maximum price to ensure that they would get paid back at the federally set maximum rate.

The figure above shows the various payment models that have been experimented with in an attempt to control costs and cut waste. The cost of the CMS programs have not just gone up year-to-year, the rate of growth has increased over time. Medicare spending increased 8.4% to $900.8 billion in 2021 accounting for 21% of the total spending on health care ($4.3 trillion). CMS estimates the total spending will increase to $6.2 trillion by 2028 with Medicare expected to show the fastest growth (7.6% increase year-over-year).
Towards a Healthcare Model that Works
One way to quantify the waste and inefficiency in the system is to create a model for health care that works and provides equivalent, if not better health outcomes, and get an estimate of what that should cost. Any health care model that works must provide for choice of doctors, and align profits with quality of care and health outcomes.
There are four distinct models [15] for providing health care – the Beveridge model, the Bismarck model, the Tommy Douglas model, and the Out-of-Pocket model.
- Beveridge model – Named after William Beveridge who created the National Health Service in the UK. In this model, the government provides health care for all citizens financed by tax payments. This ‘socialized’ model is used in the UK, Spain, Cuba, and New Zealand.
- Bismarck model – Named after Otto von Bismarck (and also called the Social Health Insurance model). In this model, employees and employers pay fees to a fund that is used to pay healthcare providers. It does not provide universal health care but covers employees who are able to pay into the scheme. The hospitals and healthcare providers are typically private institutions. The funds are considered public and insurers are not allowed to take profits. This model is used in Germany, France, Japan, and Switzerland.
- Tommy Douglas model – More commonly referred to as the National Health Insurance model and found in Canada, South Korea, and Taiwan. This model combines elements from the Beveridge and the Bismarck models, where providers are private and the government provides universal insurance and acts as the single payer for medical procedures.
- Out-of-Pocket – Found in most rural areas of the Global South in countries that do not have a national health scheme. Those who can afford it, get the care that they need.
The US healthcare model is a combination of all four models for different population segments. The Veterans Health Administration runs an integrated healthcare system similar to the Beveridge model. Employer based plans are similar to the Bismarck model (except for the fact that insurance is for-profit). Medicare available to seniors over 65 is similar to the National Health Insurance single payer model. The Out-of-Pocket model is used for the uninsured, the underinsured, and for high-deductible plans where the deductible has not been reached.
The Out-of-Pocket model is also used in the US for procedures not covered by insurance. Elective cosmetic surgery was a $14.6 billion market in the US in 2021 [16]. Without a third-party intermediating the payments, the elective cosmetic surgery market operates in a competitive free market with full price transparency, which allows consumers to shop around. The two most popular cosmetic surgeries in 2021 were liposuction and breast augmentation. The costs for both, when adjusted for inflation, have actually gone down in the last two decades [17].
In 2019, CMS introduced the Direct Contracting model (recently rebranded as ACO REACH) to address some of the issues with Medicare Advantage plans. Instead of a fee-for-service model, the Direct Contracting model puts emphasis on capitation, where a fixed payment is made for each beneficiary enrolled in the program. The Direct Contracting model is a risk-sharing arrangement with healthcare providers that provides predictable revenue to providers while requiring them to share in the risks.
To get an estimate of the waste, we will use a payment model similar to ACO REACH’s Total Care Capitation Payment model but structure it so that patients have a single touchpoint for health care. It is a risk-sharing arrangement with the healthcare providers and not tied to the volume of healthcare services provided. The payers pay directly to a primary care provider of their choice (instead of picking an insurance product) and the provider manages risk by buying insurance for specialized care. Let’s call it the Direct-Care Capitation Payment model. In this model, the only touchpoint that a patient has is their primary care provider. The primary care provider is responsible and accountable for community health outcomes.
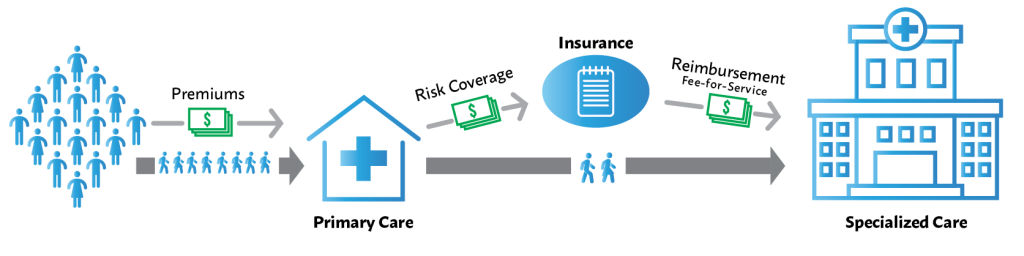
In the Direct-Care Capitation Payment model, a fixed rate is paid per family per month that covers all health care needs. The model provides predictable revenue to the primary care providers, significantly reduces administrative overheads, and eliminates claim processing. Let’s assume an average of $1000 per household per month for total health coverage paid directly to a primary care facility. A primary care facility that signs up 10,000 households will have an annual revenue of $120 million.
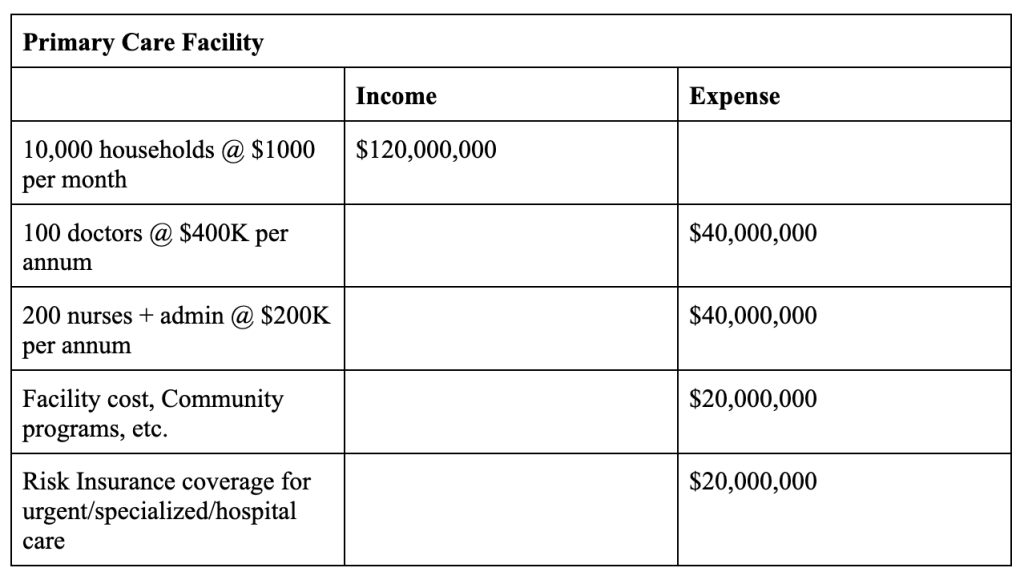
In 2022, there were about 130 million households in the US. In our model, a primary care facility caters to 10,000 households. For the entire country, that would require 13,000 primary care facilities. Each primary care facility buys $20 million in risk insurance to cover specialized care. There is a general agreement that insurance companies can keep 20% of the premiums for marketing, administrative, and overheads. In our model, since individuals do not directly buy insurance, the overheads will be significantly less. For our modeling purposes, let’s assume a 95/5 split.
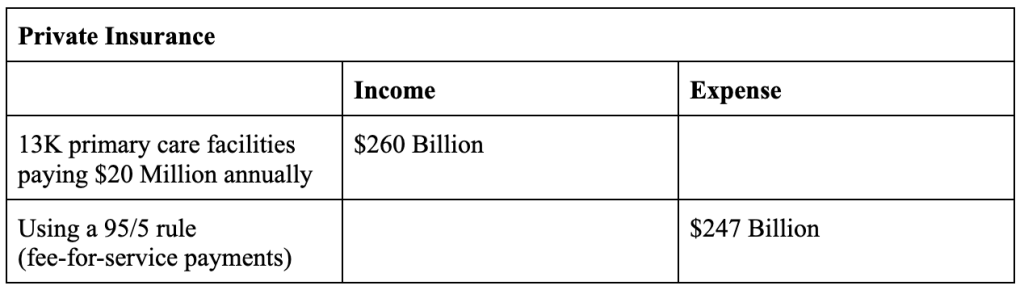

The $247 billion is paid as fee-for-service payments to the specialized care hospitals.
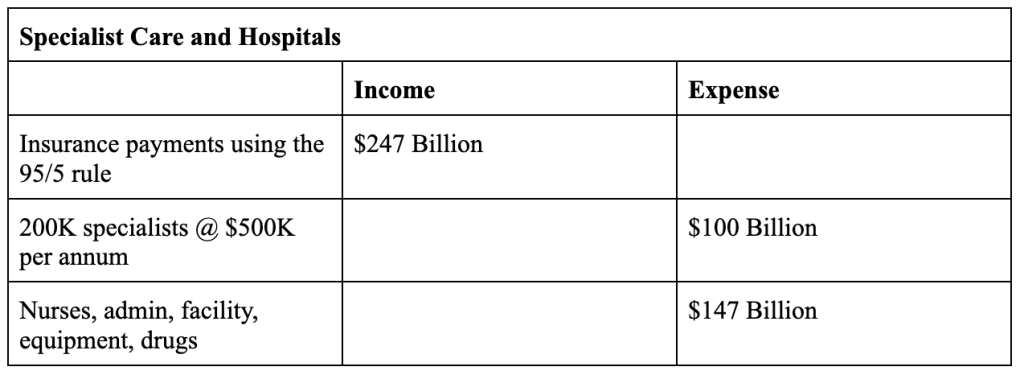
The Direct-Care Capitation Payment model will align costs with quality of care and health outcomes. Specifically, under the model,
- At open enrollment, an individual chooses a primary care facility instead of choosing an insurance product. It avoids open enrollment nightmares. The primary care facility becomes the single touchpoint for health care for a patient.
- Primary care providers buy insurance to manage risks. They are better equipped to understand risks and get appropriate coverage. The primary care facility has an incentive to keep its community healthy as it directly impacts their bottom line and they can reinvest the money back in care. Fixed and predictable revenue paid upfront allows primary care providers to provide better service and invest in infrastructure and community programs.
- Insurance company overheads are significantly lesser as they have to process fee-for-service claims only for specialist services.
- Specialist care and hospitals will continue to use the Fee-For-Service (FFS) model but fair competition will force them to innovate and lower costs which will directly impact their bottom lines.
In 2021, the US spent $4.3 trillion on health care, which accounted for around 18% of the GDP. CMS [18] estimates national health spending to grow 1.1% faster than the GDP per year on average and to reach $6.2 trillion by 2028 which will account for 19.7% of the GDP. To put this in perspective, the US spent more on health care in 2021 than the GDP of countries like Japan and Germany in 2022. In health outcomes, the US lagged behind both countries with life expectancy at a 25 year low of 76.1 years [19].
The table below compares the current US healthcare system with the Direct-Care Capitation Payment model. In this model, 13,000 primary care centers with 100 doctors each would require 1.3 million primary care physicians.
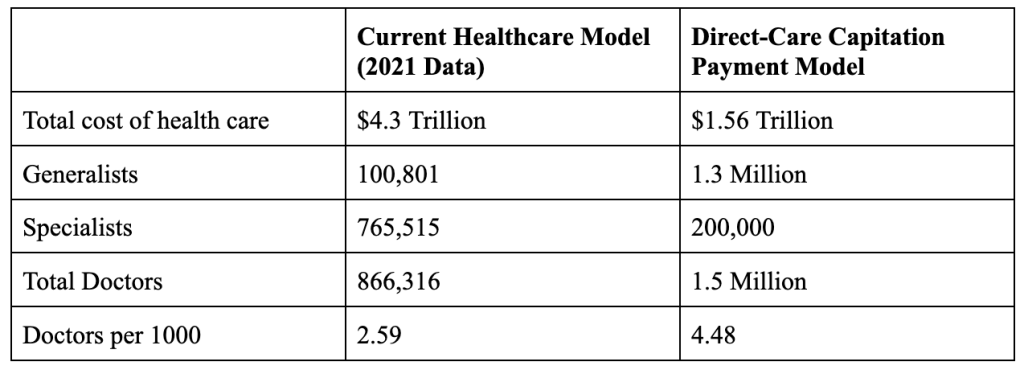
Life expectancy in the US fell in 2021 to 76.1 years, the lowest since 1996. Research [20] shows that an increase of 10 primary care physicians per 100,000 population was associated with an increase in life expectancy of 51.5 days. The Direct-Care Capitation Payment model increases the number of primary care physicians from 100,801 to 1.3 million which should show a corresponding increase in life expectancy of over 5 years.
A market-based healthcare system will weed out any specialists who order a skin biopsy for a simple rash. It will weed out providers who do unnecessary tests, the over-chargers, the over-coders, and the over-treaters. It will incentivize quality and not quantity. It will create a system where the incentive to innovate is rewarded and aligned to patient health outcomes. It will put the care back in health care.
The Secret of the Care
Health care is not a privilege. It must be recognized as a basic human right. The United Nations Sustainable Development Goal (SDG) 3 [21] requires all signatory countries to provide for universal health coverage and access to quality essential healthcare services, as well as to provide safe, effective, quality, and affordable essential medicines and vaccines for all. While not legally binding, countries are expected to take ownership and create a framework for achieving universal and affordable health care by the year 2030.
The Direct-Care Capitation Payment model will eliminate open enrollment nightmares, give you your choice of doctors, significantly reduce costs, and will improve community health outcomes. Market forces will balance the mix of generalists and specialists, align profits with quality of care and health outcomes, and allow and incentivize providers to move focus back to primary care and community health. It will prioritize quality of life over quantity of life.
In a speech [22] Dr. Francis W. Peabody gave to medical students at Harvard on October 21, 1926 he concluded with,
Time, sympathy and understanding must be lavishly dispensed, but the reward is to be found in that personal bond which forms the greatest satisfaction of the practice of medicine. One of the essential qualities of the clinician is interest in humanity, for the secret of the care of the patient is in caring for the patient.
Almost a 100 years after Dr. Peabody’s speech, we have a healthcare system where patients are shrunk-fit into 15-minute time slots, where time is too less and patients too many to form any kind of personal bond, and apps prepare the doctor for the small talk to provide the illusion of caring. It is working neither for the patient nor for the doctor. It is time for change.
References
- Anderson GF, Reinhardt UE, Hussey PS, Petrosyan V. It’s The Prices, Stupid: Why the United States Is So Different From Other Countries. Health Affairs, 22, no. 3 (2003):89-105. Available at https://www.healthaffairs.org/doi/10.1377/hlthaff.22.3.89
- Anderson GF, Hussey P, Petrosyan V. It’s Still The Prices, Stupid: Why The US Spends So Much On Health Care, And A Tribute To Uwe Reinhardt. Health Affairs, 38, no. 1 (2019). Available at https://www.healthaffairs.org/doi/10.1377/hlthaff.2018.05144
- Aetna Clinical Policy Bulletin No. 0530. Available at https://www.aetna.com/cpb/medical/data/500_599/0530.html
- Mendelson EB, Bohm-Velez M, Joseph N, Neiman HL. Gynecologic imaging: comparison of transabdominal and transvaginal sonography. Radiology 1988 166:2, 321-324. Available at https://pubs.rsna.org/doi/10.1148/radiology.166.2.3275976
- Pinder J. How much does a transvaginal ultrasound cost? $200? $421.29 Or $2165. January 16, 2022. Available at https://clearhealthcosts.com/blog/2022/01/how-much-does-a-transvaginal-ultrasound-cost-200-421-29-or-2165/
- James BC, Poulsen GP. The Case for Capitation. Harvard Business Review. July-August 2016. Available at https://hbr.org/2016/07/the-case-for-capitation
- Thompson D. Why America Has So Few Doctors. The Atlantic. February 14, 2022. Available at https://www.theatlantic.com/ideas/archive/2022/02/why-does-the-us-make-it-so-hard-to-be-a-doctor/622065/
- Abelson R, Sander-Katz M. ‘The Cash Monster Was Insatiable’; How Insurers Exploited Medicare for Billions. New York Times. October 08, 2022. Available at https://www.nytimes.com/2022/10/08/upshot/medicare-advantage-fraud-allegations.html
- Langreth R, Ingold D, Gu J, The Secret Drug Pricing System Middlemen Use to Rake in Millions. Bloomberg, September 11, 2018. Available at https://www.bloomberg.com/graphics/2018-drug-spread-pricing/
- Trish EE, Nuys KV, Popovian R. PBMs are inflating the cost of generic drugs. They must be reined in. Stat News. June 30, 2022. Available at https://www.statnews.com/2022/06/30/pbms-inflating-cost-generic-drugs/
- Morrison C. America’s Most Expensive Drugs Revealed. Daily Mail Online. December 28, 2022. Available at https://www.dailymail.co.uk/health/article-11547237/Americas-expensive-drugs-revealed-insurers-pay-these.html
- Engelberg A. Unaffordable prescription drugs. The real legacy of the Hatch-Waxman Act. Stat News. December 16, 2020. Available at https://www.statnews.com/2020/12/16/unaffordable-prescription-drugs-real-legacy-hatch-waxman-act/
- Swift T. Bad Blood. 1989, Big Machine, 2014. Available at https://youtu.be/QcIy9NiNbmo
- HealthCare.gov. Rate Review and the 80/20 Rule. Available at https://www.healthcare.gov/health-care-law-protections/rate-review/
- Wallace LS. A view of health care around the world. Ann Fam Med. 2013 Jan-Feb;11(1):84. doi: 10.1370/afm.1484. PMID: 23319511; PMCID: PMC3596027. Available at https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3596027/
- The Aesthetic Society. Aesthetic Plastic Surgery National Databank Statistics 2020-2021. Available at https://cdn.theaestheticsociety.org/media/statistics/2021-TheAestheticSocietyStatistics.pdf
- Perry MJ. What Economic Lessons about Health Care Costs Can We Learn from the Competitive Market for Cosmetic Procedures. AEI. Available at https://www.aei.org/carpe-diem/what-economic-lessons-about-health-care-costs-can-we-learn-from-the-competitive-market-for-cosmetic-procedures-2/
- NHE Fact Sheet. Centers for Medicare and Medicaid Services. Available at https://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/NationalHealthExpendData/NHE-Fact-Sheet
- Lewis T. Why Life Expectancy Keeps Dropping in the U.S. as Other Countries Bounce Back. Scientific American. November 21, 2022. Available at https://www.scientificamerican.com/article/why-life-expectancy-keeps-dropping-in-the-u-s-as-other-countries-bounce-back1/
- Basu S, Berkowitz SA, Phillips RL, Bitton A, Landon BE, Phillips RS. Association of Primary Care Physician Supply With Population Mortality in the United States, 2005-2015. JAMA Intern Med. 2019 Apr 1;179(4):506-514. doi: 10.1001/jamainternmed.2018.7624. PMID: 30776056; PMCID: PMC6450307. Available at https://pubmed.ncbi.nlm.nih.gov/30776056/
- United Nations Department of Economic and Social Affairs. The 17 Sustainable Development Goals. Available at https://sdgs.un.org/goals
- Peabody FW. The Care of the Patient. JAMA. 1927;88(12):877-882. doi:10.1001/jama.1927.02680380001001. Available at https://jamanetwork.com/journals/jama/article-abstract/245777
Acknowledgements
I would like to acknowledge the use of the Hawkai Data platform (https://hawkai.net/) in analyzing and visualizing the data. For any questions regarding this article, you can email me at raina.john1@gmail.com.
OECD data is available at https://stats.oecd.org/
CMS data is available at https://data.cms.gov/
Learn more about Hawkai Data at https://hawkai.net, follow us on LinkedIn at https://www.linkedin.com/company/hawkai-data/, or talk to us at info@hawkai.net.